Why Are Wounds Harder to Heal in Winter?
1. Weakened Skin Barrier Function
Cold and dry winter air reduces sebum production, leading to dehydration of the stratum corneum. This causes cracks and micro-lesions that serve as entry points for bacteria.
2. Slower Blood Circulation
Low temperatures constrict peripheral blood vessels, reducing oxygen and nutrient delivery to tissues. This slows down cellular activity essential for wound healing, such as fibroblast and keratinocyte function.
3. Reduced Immune Response
During winter, metabolic activity and vitamin intake decrease, which lowers immune cell activity and increases infection risk.
4. Increased Friction from Clothing
Thick clothing, tight shoes, or boots can cause unnoticed skin friction or pressure injuries, which become difficult to heal under repeated irritation.

Key Strategies for Winter Wound Management
1. Maintain a Moist Healing Environment (Moist Wound Healing)
In dry air, traditional gauze dressings can cause scabbing and cracking.
Recommended: Hydrocolloid or Hydrogel Dressings
These dressings can:
* Maintain optimal moisture to promote cell migration;
* Absorb exudate and prevent secondary infection;
* Reduce dressing change frequency, minimizing wound exposure.
2. Choose Dressings with Both Warmth and Breathability
Winter wound dressings should retain warmth without trapping moisture.
* Multi-layer hydrocolloid dressings with a waterproof PET film, absorbent middle layer, and hydrocolloid matrix base are ideal.
* Recommended for: Knees, ankles, and hands—areas prone to exposure or friction.
3. Strengthen the Skin Barrier
For dry or cracked skin, use repair patches containing hydrocolloid or silicone to reduce transepidermal water loss.
4.Prevent Cold-Induced Circulatory Issues
For patients with diabetic foot ulcers or poor peripheral circulation, maintaining warmth is crucial. Gentle heat therapy or massage can support local blood flow.
5.Nutritional Support
Adequate intake of vitamin C, protein, and zinc promotes collagen synthesis and tissue repair.
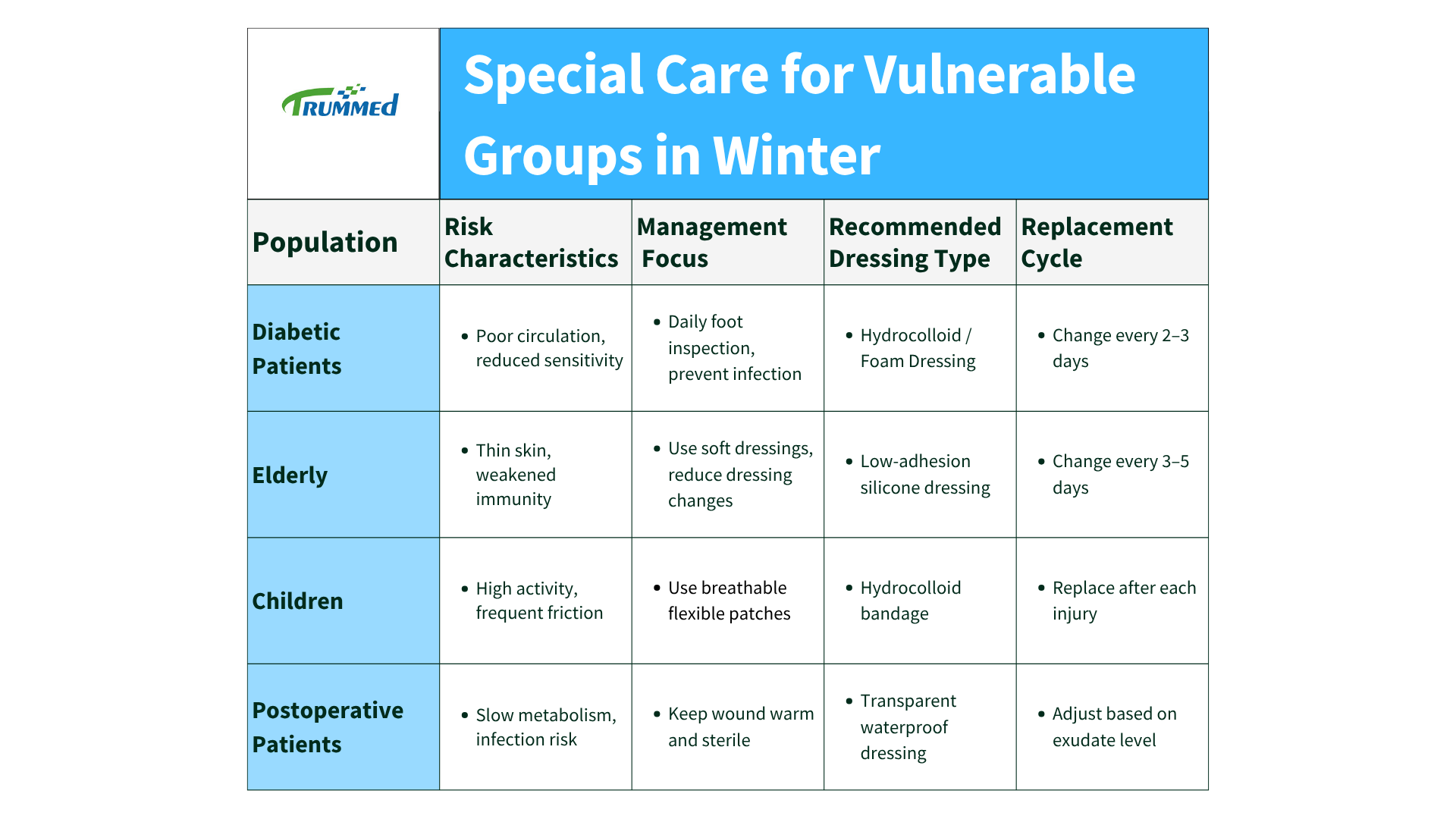
Emerging Trends in Winter Wound Care
1. Smart Temperature-Sensing Dressings
These can detect local temperature changes to identify infection risks early.
2. Hydrocolloids with Natural Moisturizing Ingredients
Infused with hyaluronic acid, honey extract, or alginates, combining hydration and antibacterial protection.
3. Low-Allergy, High-Adhesion Silicone Dressings
Ideal for patients with sensitive or allergy-prone skin.
Conclusion
-The essence of winter wound management lies not in “how often you c hange the dressing,” but in “how well you maintain moisture, warmth, and barrier integrity.”
Modern hydrocolloid dressings not only accelerate wound healing but also prevent dryness, infection, and scarring.
In the cold season, “let the skin heal in moisture and warmth” — that is the true science of care.






